Molluscum Contagiosum
- Molluscum contagiosum is a rare viral infection that is exclusive to humans. It is characterised with the presence of small elevated lesions called papules. These papules have a waxy surface and are seen on various parts the body such as the face, trunk, arms and legs. It can also affect the armpits but does not involve the palms. It has also been found to affect the eyelids.
-
In this article, we shall discuss molluscum contagiosum in a bit more detail.
Cause of molluscum contagiosum
Molluscum contagiosum is caused by a viral infection. The portal of entry of the riders into the body is usually through some form of break in the skin. This occurs through direct skin to skin contact as well and can therefore be seen in individuals who share showers or athletes who share equipment in the gym.
Having low levels of immunity such as in the case of HIV virus infections can also make an individual prone to developing molluscum contagiosum. In such individuals, the lesions are a lot more widespread. In children, the condition occurs due to sharing of towels and sponges. Studies have also shown the development of molluscum contagiosum affecting the eyelids of both eyes following treatment of rheumatoid arthritis with specialist drugs such as methotrexate. Case studies have reported the eyelids being affected in children.
Clinical features of molluscum contagiosum
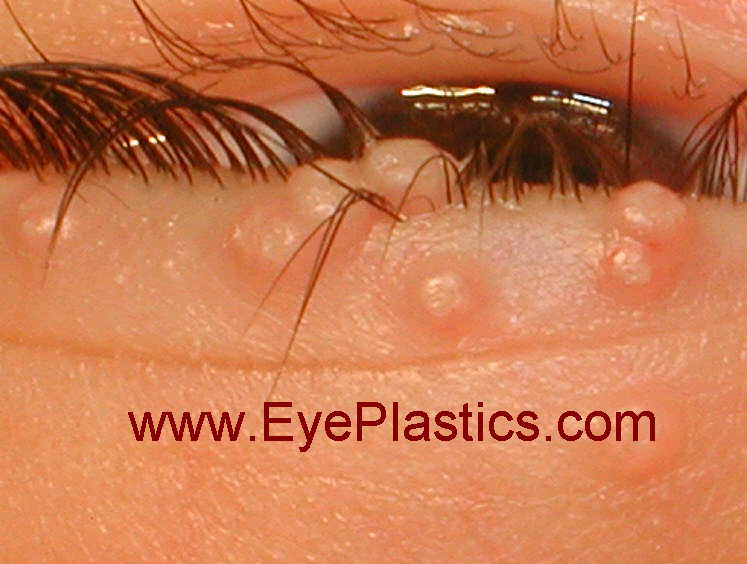
Typically, molluscum contagiosum results in the formation of multiple small papules with a waxy surface. They might be clearly evident on the body especially on the eyelids. Typically, scratching the lesions can make them worse as more and more lesions form along the line of scratching. This is a typical phenomenon called as Koebner phenomenon
.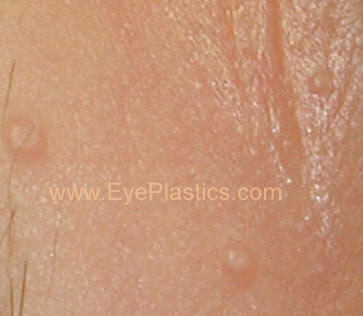
Upon examination, the lesions are flesh coloured and vary between 2 to 5 mm in size. Patients with poor immune levels tend to have multiple lesions all over the body. The involvement of the eyelids and the face is commonly seen in children whereas the involvement of the groin area is seen in adults. Associated with molluscum contagiosum are other skin conditions such as atopic dermatitis and eczema.
Diagnosis of molluscum contagiosum
A diagnosis of molluscum contagiosum can be made by tests such as polymerase chain reaction and biopsy. A biopsy demonstrates the presence of specific structures within the lesions called inclusion bodies. These bodies can be stained using specific stains to help identify them under a microscope.
Treatment of molluscum contagiosum
Most cases of molluscum contagiosum tend to resolve themselves in a few months. Molluscum contagiosum that affect the eyelids might be managed conservatively without performing any intervention. However frequently, a small amount of trauma to the lesion can help get rid of it. Another form of treatment is called curettage and involves administration of an anaesthetic agent followed by removal of the lesion completely.
Medical treatment is also available to manage molluscum contagiosum. However, detailed studies have shown that there does not appear to be any additional benefit of using these treatments (skin creams, anti-viral agents and herbal medicines) when compared to not offering the patient any treatment whatsoever.
Following the treatment, patients might require follow-up appointments to see if the lesion is recurring.
Conclusion
Molluscum contagiosum is an uncommon problem that can affect various parts of the body. The involvement of the eyelids is more often seen in children and usually resolves by itself. Specific treatments can be offered though recurrence rates can be high.
Molluscum contagiosum (MC) is a viral infection of the skin or occasionally of the mucous membranes. It is caused by a DNA poxvirus called the molluscum contagiosum virus (MCV). MCV has no animal reservoir, infecting only humans. There are four types of MCV, MCV-1 to -4; MCV-1 is the most prevalent and MCV-2 is seen usually in adults and often sexually transmitted. This common viral disease has a higher incidence in children, sexually active adults, and those who are immunodeficient, and the infection is most common in children aged one to ten years old.MC can affect any area of the skin but is most common on the trunk of the body, arms, and legs. It is spread through direct contact or shared items such as clothing or towels.
The virus commonly spreads through skin-to-skin contact. This includes sexual contact or touching or scratching the bumps and then touching the skin. Handling objects that have the virus on them (fomites), such as a towel, can also result in infection. The virus can spread from one part of the body to another or to other people. The virus can be spread among children at day care or at school. Molluscum contagiosum is contagious until the bumps are gone-which, if untreated, might be up to 6 months or longer.
The time from infection to the appearance of lesions can range up to 6 months, with an average incubation period between 2 and 7 weeks.
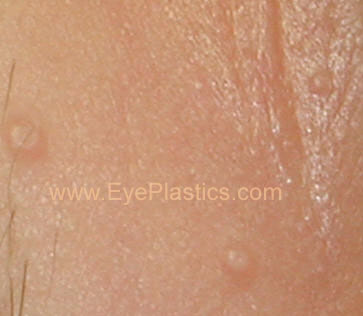
Diagnosis is made on the clinical appearance; the virus cannot routinely be cultured. The diagnosis can be confirmed by excisional biopsy.
Histologically, molluscum contagiosum is characterized by molluscum bodies in the epidermis above the stratum basale, which consist of large cells with:
- abundant granular eosinophilic cytoplasm (accumulated virons), and
- Symptoms
Molluscum contagiosum lesions are flesh-colored, dome-shaped, and pearly in appearance. They are often 1–5 millimeters in diameter, with a dimpled center. They are generally not painful, but they might itch or become irritated. Picking or scratching the bumps might lead to further infection or scarring. In about 10% of the cases, eczema develops around the lesions. They might occasionally be complicated by secondary bacterial infections. In some cases the dimpled section might bleed once or twice. The viral infection is limited to a localized area on the topmost layer of the epidermis. Once the virus containing head of the lesion has been destroyed, the infection is gone. The central waxy core contains the virus. In a process called autoinoculation, the virus might spread to neighboring skin areas. Children are particularly susceptible to auto-inoculation, and might have widespread clusters of lesions.
.png)